Extruded disc herniation is a common spinal condition that affects millions of people worldwide. This medical issue occurs when the soft inner core of a spinal disc protrudes through the tough outer layer, causing pain and discomfort, and potentially impacting one's overall quality of life. Severe cases of disc herniation may require surgical intervention where the surgeon may apply Spine implants. In this blog post, we will delve into the intricacies of extruded disc herniation, exploring its causes, symptoms, and available treatment options.
0 Comments
In the ever-evolving landscape of healthcare, diagnostic imaging has emerged as a cornerstone in various medical specialties, notably in the field of orthopedics. As technological advancements continue to reshape the way we approach patient care, diagnostic imaging stands out as an invaluable tool, providing crucial insights into musculoskeletal conditions. It also assists in decision-making whether Orthopedic Implants are required for the treatment or not. And if required, what type of implant will be needed? This blog explores the pivotal role of diagnostic imaging in orthopedics and its contribution to precision medicine.
Orthopedics – An IntroductionOrthopedics, the branch of medicine focused on the musculoskeletal system, involves the diagnosis and treatment of conditions affecting bones, joints, muscles, ligaments, and tendons. Traditionally, orthopedic assessments heavily relied on physical examinations and patient histories. However, the advent of diagnostic imaging has revolutionized the diagnostic process by allowing clinicians to visualize the internal structures of the musculoskeletal system. Various Imaging ModalitiesSeveral imaging modalities play a significant role in orthopedics, each offering unique advantages depending on the nature of the condition. X-rays are often the first line of defense, providing detailed images of bones to diagnose fractures, arthritis, and other skeletal abnormalities. Magnetic Resonance Imaging (MRI) offers a more comprehensive view, excelling in capturing soft tissue details such as ligaments, tendons, and cartilage. Computed Tomography (CT) scans, on the other hand, excel in creating detailed cross-sectional images, aiding in the assessment of complex fractures and spinal conditions. Precision Diagnosis and Treatment PlanningDiagnostic imaging in orthopedics goes beyond mere visualization; it plays a pivotal role in precision medicine. Accurate and detailed images enable orthopedic specialists to formulate tailored treatment plans based on an individual's unique anatomy and pathology. From planning surgical procedures to determining the most effective rehabilitation strategies, diagnostic imaging empowers healthcare providers to deliver personalized care that optimizes outcomes and minimizes potential risks. Early Detection and PreventionOne of the most significant contributions of diagnostic imaging to orthopedics is its ability to facilitate early detection and prevention of musculoskeletal disorders. Identifying issues in their nascent stages allows for timely intervention, preventing the progression of conditions and minimizing the impact on a patient's quality of life. Whether it's identifying stress fractures in athletes or detecting the early signs of arthritis, diagnostic imaging acts as a powerful preventive tool. Monitoring Treatment ProgressIn addition to aiding in diagnosis and treatment planning, diagnostic imaging is instrumental in monitoring the progress of orthopedic treatments. Follow-up imaging allows healthcare providers to assess the effectiveness of interventions, making adjustments as needed. This iterative approach ensures that patients receive optimal care throughout their orthopedic journey, with the ability to adapt treatments based on real-time feedback from diagnostic images. ConclusionThe role of diagnostic imaging in the field of orthopedics cannot be overstated. It has transformed the landscape of musculoskeletal medicine, providing a window into the intricate structures of the human body. From precise diagnosis and personalized treatment planning to early detection and progress monitoring, diagnostic imaging is at the forefront of delivering quality orthopedic care. As technology continues to advance, the synergy between diagnostic imaging and orthopedics will undoubtedly usher in new possibilities, further enhancing our ability to understand, diagnose, and treat musculoskeletal conditions with unprecedented precision. Unveil the future of orthopedics and experience live demonstrations of the latest healthcare products and technologies at the 48th Annual Conference Odisha (OOACON). Orthopedic injuries and conditions have long been a significant source of pain and discomfort for many people. Traditional treatment methods often involve surgical procedures involving Orthopedic implants or the use of pain medications, which may not always provide lasting relief. However, recent advancements in medical science have brought forth a promising solution: regenerative therapy in orthopedics. This innovative approach is revolutionizing the field, offering patients an opportunity to heal naturally and effectively.
Understanding Regenerative Therapy Regenerative therapy, also known as regenerative medicine, is a cutting-edge branch of medical science that focuses on harnessing the body's innate ability to repair and regenerate damaged tissues. In orthopedics, this therapy involves using a patient's own cells or biologically active substances to stimulate healing and tissue regeneration in joints, tendons, ligaments, and bones. This approach holds great promise as it not only addresses the symptoms but also targets the root causes of orthopedic issues. Types of Regenerative Therapies Platelet-Rich Plasma (PRP) Therapy PRP therapy involves drawing a small amount of the patient's blood, processing it to concentrate platelets, and then injecting this PRP back into the injured area. Platelets contain growth factors that help stimulate tissue repair and reduce inflammation. This therapy is commonly used for conditions such as tendonitis and osteoarthritis. Stem Cell Therapy Stem cells are undifferentiated cells that can develop into various types of tissue. In orthopedics, stem cell therapy typically involves harvesting stem cells from the patient's own bone marrow or fat tissue and injecting them into the injured area. These stem cells promote tissue repair and regeneration, making them valuable for treating conditions like cartilage defects and joint injuries. Amniotic Fluid and Tissue Amniotic fluid and tissue contain a rich source of growth factors and proteins that can aid in tissue repair and regeneration. These substances are obtained from donated amniotic tissue, ensuring that patients do not need to rely on their own cells for treatment. Amniotic regenerative therapy is a non-invasive option used for joint pain and tendon injuries. Benefits of Regenerative Therapy Natural Healing One of the primary advantages of regenerative therapy is that it leverages the body's natural healing processes. This reduces the risk of adverse reactions and complications that can be associated with synthetic medications or invasive surgical procedures. Minimally Invasive Regenerative treatments are often administered through injections, making them minimally invasive compared to surgical alternatives. Patients experience less pain, shorter recovery times, and reduced scarring. Targeted Treatment Regenerative therapy addresses the underlying causes of orthopedic issues, rather than merely masking the symptoms. This can provide long-lasting pain relief and improved joint function. Low Risk of Rejection Since many regenerative therapies use the patient's own cells or amniotic materials, there is a low risk of rejection or adverse reactions. Future of Regenerative Therapy in Orthopedics As regenerative therapy in orthopedics continues to evolve, it holds immense potential for further advancements. Research is ongoing to refine techniques and expand the range of conditions that can be effectively treated using these methods. This includes exploring the potential of 3D bioprinting to create custom tissues and cartilage, as well as developing more precise delivery methods for regenerative treatments. To Know more about advancements in the field of orthopedics and understand the latest treatment approaches, register for the 43rd SICOT Orthopaedic World Congress. A fracture is a break in a bone. It can be caused by trauma, such as a fall, car accident, or sports injury, or by overuse. Fractures can also be caused by diseases that weaken bones, such as osteoporosis. Severe fractures often need surgery and this may also involve the use of a Locking Plate System or other trauma implants depending on the type and severity of the fracture.
Fracture healing is a complex process that takes several weeks or months to complete. The first step in healing is the formation of a blood clot at the fracture site. This blood clot provides a scaffold for new bone cells to grow on. Over the next few weeks, the blood clot is replaced by a soft callus, which is made up of cartilage and fibrous tissue. The callus holds the fractured bones together and provides a framework for new bones to form. Over the next few months, the callus is hardened by the deposition of calcium and other minerals. This process is called ossification. Once the callus has hardened, it is remodeled to match the shape and strength of the original bone. How long it takes for a fracture to heal depends on a number of factors, including the type of fracture, the location of the fracture, the person's age and overall health, and whether or not there are any complications. How to Identify Fracture Healing? There are a number of ways to identify fracture healing. The most common way is to monitor the person's symptoms. As the fracture heals, the pain and swelling should gradually decrease. The person should also be able to move the injured area more easily. Another way to identify fracture healing is to have X-rays taken of the fracture site. X-rays can show the formation of new bone and the remodeling process. In some cases, the doctor may order other tests, such as a CT scan or MRI, to get a better look at the fracture site. Signs and Symptoms of Fracture Healing Some of the signs and symptoms of fracture healing include:
Factors that Can Affect Fracture Healing There are a number of factors that can affect fracture healing, including: Type of fracture: Some fractures, such as simple breaks, heal more quickly than others, such as comminuted fractures (fractures that involve multiple breaks in the bone). Location of fracture: Fractures that occur in areas with a good blood supply, such as the long bones of the arms and legs, tend to heal more quickly than fractures that occur in areas with a poor blood supply, such as the hip and pelvis. Person's age and overall health: Younger people and people with good overall health tend to heal from fractures more quickly than older people and people with chronic health conditions. Complications: Complications, such as infection and nonunion (failure of the fracture to heal), can delay fracture healing. What to do to help your fracture heal? There are a number of things you can do to help your fracture heal, including:
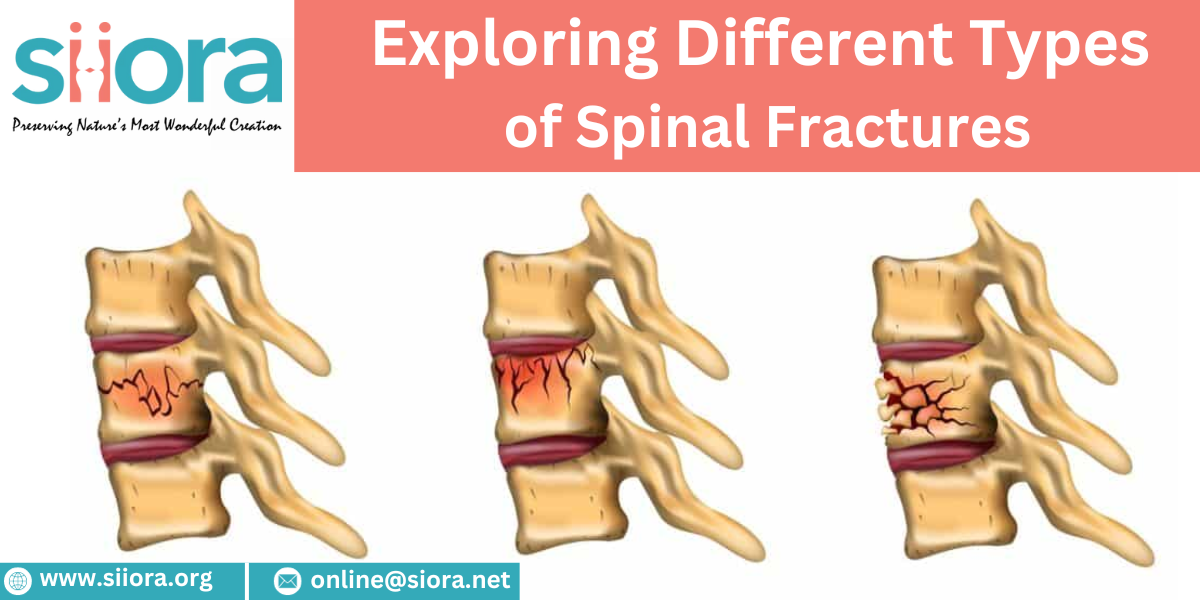
To know about the advancements in the orthopedic industry and participate in lectures, scientific papers, and presentations at an international event, register for the Orthopaedic World Congress in Egypt. The human spine is a remarkable and complex structure that provides support, stability, and flexibility to our bodies. Unfortunately, accidents, falls, and other traumatic events can lead to spinal fractures, which can have significant consequences for an individual's health and mobility. This blog will delve into the various types of spinal fractures, shedding light on their causes, symptoms, and potential treatments. Find experienced trauma implant manufacturers to get an international standard quality range of Titanium Spinal Implants.
|
ArchivesCategories |




 RSS Feed
RSS Feed
